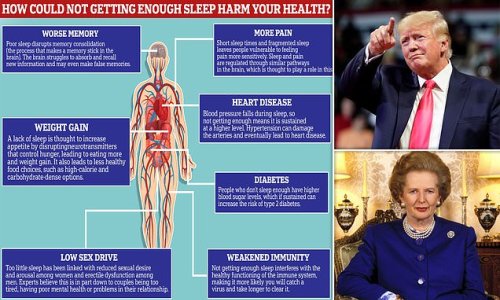
(Daily Mail) Functioning on a measly four hours of sleep a night used to be a badge of honour for high-powered CEOs and world leaders.
Part of Margaret Thatcher’s fearsome reputation came from how little she slept. Donald Trump used to brag that some nights he would only get three hours.
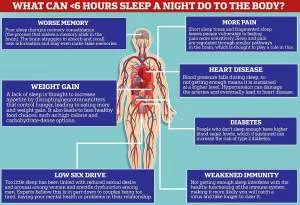
But a wealth of scientific studies in recent years have unequivocally shown that not getting enough shut eye can lead to a host of life-threatening diseases.
Yet two-thirds of adults throughout all developed nations fail to get the recommended eight hours.
There is a tiny subset of the population — about one in 4million of us — born with a gene that allows them to thrive on half of that amount.
But for the vast majority, routinely sleeping less than six or seven hours a night demolishes your immune system and significantly raises your risk of developing numerous forms of cancer.
A study of 60,000 middle-aged and elderly Britons, published this week, found those who regularly need to nap during the day were 12 per cent more likely to develop high blood pressure than their peers.
The researchers concluded the naps themselves were not the problem, and suggested they were a sign of poor quality sleep at night.
Even moderate reductions in sleep for just a week can disrupt blood sugar so profoundly you would be classified as pre-diabetic.
Sleep deprivation also increases the risk of your coronary arteries becoming blocked and brittle, setting you on a path towards cardiovascular disease, stroke or heart failure.
Maybe you’ve noticed you crave junk food when you’re tired? Too little sleep swells concentrations of a hormone that makes you feel hungry, while suppressing a hormone that tells you you’re satisfied.
Sleep also seems to be a key lifestyle factor that determines whether or not you will develop Alzheimer’s disease — with getting too much or not enough both linked to the disease.
Sleep disruption may also contribute to major psychiatric conditions, including depression and anxiety. It has even been linked to suicide.
So, how do you know whether you’re routinely getting enough sleep? A good rule of thumb is to ask yourself if you could fall back asleep at 10am or 11am. If the answer is yes, you are probably not getting the sufficient quantity and/or quality of sleep.
Cancer
Routinely not getting enough sleep has been linked to greater ‘wear and tear’ on our cells. This type of disruption to our genes is thought to give rise to cancerous tumours.
A 2019 study found people who work night shifts have 30 per cent more damage to their DNA compared to those who work normal hours.
In a 2010 study, researchers in Ohio linked sleeping less than six hours a night to a 50 per cent increased risk of bowel cancer.
With this type of cancer being the second deadliest in the UK and US, the Case Western Reserve University study concluded that short sleep is a ‘public health hazard’.


In addition to DNA damage, insufficient sleep may affect cancer by suppressing levels of key hormones in the body.
Melatonin is key to making us feel sleepy. Throughout the day, levels of the hormone remain very low in the body but as the day wears on, its production increases and the end result is that you feel tired.
But melatonin levels can be suppressed by not enough or fragmented sleep.
A lack of sleep may also indirectly heighten cancer risk – by making us hungrier and fatter.
In 2012, research published in the journal PLoS One looked at the cancer risk in nearly 25,000 middle-aged adults across Europe.
Itfound people who slept less than six hours per night were 43 per cent more likely to develop cancer in their lifetime than those who got seven or more hours.
A separate 2019 study found patients who slept six or less hours a night were nearly three times more likely to die from cancer within 30 years than those who got seven hours or more.
Researchers from Penn State University looked at 1,654 adults aged 20 to 74 who had a history of heart disease or stroke.
Those who were sleep deprived had a 2.92-times greater risk of dying from any cancer within three decades than those who got sufficient rest, according to the paper published in the Journal of the American Heart Association.
Heart problems
The link between an unhealthy sleeping pattern and an unhealthy heart is becoming undeniable.
As we approach midlife, and our body and health begin to deteriorate, the impact of insufficient sleep on the cardiovascular system escalates.
Adults aged 45 or older who sleep fewer than six hours a night are 200 per cent more likely to have a heart attack or stroke during their lifetime, compared with those sleeping seven to eight hours a night.
This finding, from a 2012 study by Chicago University, emphasises how important it is to prioritise sleep in midlife — which is unfortunately the time when family and professional circumstances encourage us to do the exact opposite.
It doesn’t take much sleep deprivation to impact your cardiovascular system. One night of modest sleep reduction — even just one or two hours — will promptly speed the contracting rate of a person’s heart, hour upon hour.
This also causes a significant increase in systolic blood pressure, which puts greater strain on the heart and blood vessels.
You will find no solace in the fact that the experiments that confirmed this were conducted in young, fit individuals, all of whom started out with an otherwise healthy cardiovascular system just hours before.
Beyond accelerating your heart rate and increasing your blood pressure, a lack of sleep damages those strained blood vessels.
The coronary arteries, which supply the heart with blood, are especially affected. These need to be clean and stay open wide at all times.
If these passageways are narrowed or blocked, your heart can suffer a comprehensive — and often fatal — attack caused by blood oxygen starvation.

One cause of a coronary artery blockage is atherosclerosis, where hardened plaques which contain calcium deposits build up in the arteries.
There is also a yearly ‘global experiment’ that involves 1.5 billion people and highlights the link between a poor night of sleep and our heart health.
In the Northern Hemisphere, the switch to daylight saving time in March results in most people losing an hour of sleep.
Researchers have tabulated millions of hospital records and discovered that this seemingly trivial sleep reduction comes with a frightening spike in heart attacks the following day.
It works both ways. In the autumn, rates of heart attacks plummet the day after the clocks go back, when we gain an hour of sleep.
A similar rise-and-fall relationship can be seen with the suicide rate, as well as the number of traffic accidents.
This proves that the brain, by way of attention lapses, microsleeps and emotional instability, is just as sensitive as the heart to very small disruptions in sleep.